 🖨️ Print post
🖨️ Print post
Appropriate Pre- and Post-Extraction Protocols When Surgical Intervention is Necessary
The decision to pull a tooth is a very important and permanent one. It requires the active participation of the patient, the holistic physician/practitioner, and the biological dentist. If tooth extraction (or surgery of a former extraction site) is deemed necessary, individuals greatly enhance their chances of a positive outcome by adhering closely to pre- and post-cavitation surgery protocols.
A dental “focus” is defined as an area anywhere in the mouth— whether a tooth or an extraction site—that is chronically irritated and/ or infected. These “dental focal infections” can include impacted wisdom teeth, incompletely extracted wisdom (and other) teeth, failed root canals, failed dental implants, and devitalized teeth (from deep fillings, crowns or physical trauma). What makes chronic dental focal infections so particularly difficult to diagnose is their relative silence in the mouth. That is, in contrast to acute illnesses such as ear infections that can feel quite fiery and hot, typically dental foci “smolder” for years, manifesting only mild and intermittent symptoms of pain and swelling.
DENTAL FOCI AND DISTURBED FIELDS
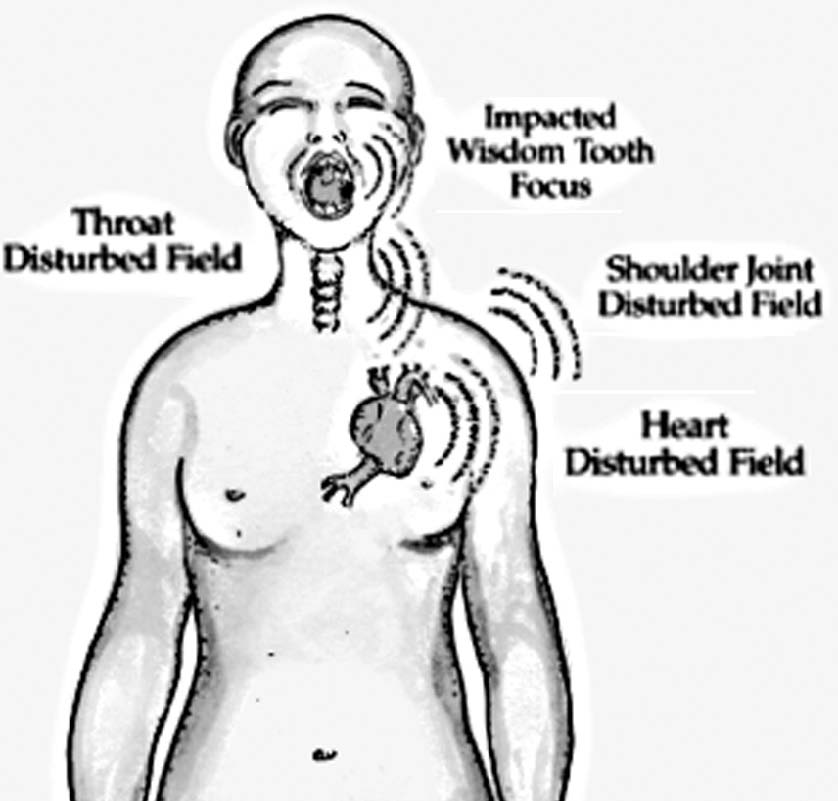
However, what is not silent are the “disturbed fields” which these dental focal infections typically cause in the body. For example, although a left lower (number 17) impacted wisdom tooth may manifest no significant pain or inflammation locally, the patient may be quite aware of distal symptoms related to this site. Chronic left shoulder pain and/or intermittent heart pain and palpitations are classic signs and symptoms of the disturbed fields secondary to this chronic dental focal infection (Figure 1).

Figure 1
Note that these symptoms are also ipsilateral; that is, on the same side as the dental focus. If, for example, a patient complains of chronic right-sided symptoms such as writer’s cramp (wrist tendonitis), right hip or shoulder pain, and right sciatica, a knowledgeable doctor or practitioner would first want to rule out an ipsilateral—that is, right-sided—dental focal infection (Figure 2). This tendency of dental foci to cause ipsilateral disturbed fields is therefore an excellent diagnostic clue that can be used in helping to determine the primary cause of a patient’s particular chronic one-sided symptoms.

Figure 2
CONSERVATIVE BIOLOGICAL DENTISTRY
Good dentists do everything possible to try to save a tooth. They don’t recommend extraction—or even a root canal—until all other avenues of treatment have been exhausted. These can include ozone injections to try to heal infection in the tooth, laser treatments, isopathic remedies (Notatum 4X, Aspergillus 4x, etc.), and nutritional support (ubiquinol/CoQ10, crystal sulfur/MSM, Schuessler’s cell salts, original Quinton Marine Sea Plasma, etc.).
Additionally, both biological dentists and holistic physicians and practitioners endeavor to first adequately diagnose what’s wrong with the tooth (or socket) in order to determine the underlying problem. For example, if a patient is eating excessive sugar this could be the true cause of pain and inflammation manifesting in a first molar. This tooth has a reflexive relationship with the pancreas and stomach. By changing one’s diet (and nothing is more motivating than the thought of a root canal or the loss of a tooth) to a nutrient-dense one and avoiding refined sugar, along with supportive nutritional supplementation, the first molar can often be saved.
It should also be noted that it is essential in most cases to clear the teeth of any toxic dental materials such as mercury amalgam, and aluminum and nickel in conventional porcelain and gold crowns, before extracting teeth. Clearing the mouth of these heavy metals often removes a galvanic dental focus. This term refers to the intermittent pain or irritation (or no local symptoms) induced in a tooth from two different metals placed on or near a tooth.
DENTAL GALVANIC FOCI
Dental galvanism, or electrogalvanism, can even occur from just one amalgam filling since these fillings themselves are a mixture of mercury, silver, copper, tin and zinc. However, galvanic dental foci typically arise from a highly positively charged gold crown placed on or near a highly negatively charged mercury amalgam filling. When mercury makes contact with gold in the mouth, a galvanic cell or “dental battery” is formed, with a current running between the mercury (functioning as an anode) and the gold (functioning as a cathode). The resulting anodic corrosion of mercury in these dental batteries has been measured at ten to twenty times higher than corrosion in a single amalgam filling alone.
As previously described, these strong electrical currents that create a dental galvanic focus can be relatively asymptomatic locally, but refer pain to distal parts of the body (ipsilateral disturbed fields), or they can cause intermittent mild irritation or pain in the tooth itself and surrounding gums. Unfortunately many dentists misdiagnose galvanic pain and refer patients to endodontists for a root canal. This is very disturbing to see in a patient’s history since these galvanic foci could have been cleared conservatively by simply replacing the gold and mercury with metal-free alternative dental materials, and thus saving the tooth.
Therefore, if your dentist recommends a root canal for a sore or painful tooth, it is essential to get a second opinion. In fact, the ready recommendation of a root canal should be a red flag for any patient to seriously consider changing from a conventional dentist to a biological (holistic) one. Your health—and even your life—depend on it.
HIGH QUALITY X-RAYS ESSENTIAL
A periapical view, which is a specific x-ray of the root of the tooth in question, is essential to diagnosis. If there is a clear radiolucency at the root of the tooth; that is, a black circular area, this is an indication of a cavitation or hole in the jawbone. This area of chronic ischemia (lack of blood supply) and infection is referred to by various terms (osteonecrosis, osteomyelitis, NICO, etc.), but broadly speaking it is a dental focal infection. When there is an obvious radiolucency apparent on x-ray there is very little one can do to save the tooth, although some dentists have been able to reduce and even clear very small cavitation areas through ozone injections. However, in most cases, when the x-ray is positive, the decision whether to do a root canal or extract the tooth then needs to be made.
If the periapical view of the tooth is negative; that is, no black radiolucency or other signs are apparent, then the biological dentist and physician endeavor to do everything possible to save the tooth with holistic therapies and supplements. However, it is important to remember that x-rays are not always definitive in determining dental foci. In fact, radiological evidence of a bone cavitation area is not even visible until as much as thirty to fifty percent of the jawbone is destroyed.1 So if symptoms continue despite holistic care, further imaging studies may be appropriate such as a 3-D Cone Beam Scanner, which uses digital technology to record images, revealing much more than simple “flat” x-rays.
ROOT CANAL OR EXTRACTION?
The irreversible decision of whether to have a root canal or extraction should only be made when both the dentist and doctor have exhausted all conservative measures to try to reduce the infection and save the tooth. When these efforts have failed over time, the first decision a patient must face is whether to have a root canal procedure or to extract the tooth. Dr. Weston A. Price, the quintessential holistic physician, always weighed the state of the tooth against the health of the patient: “. . . all pulpless teeth, root filled or not, harbor so much danger of becoming infected that they should be extracted, though the time as to when they should be extracted will depend on several contributing factors. If the patient belongs to a family in which there is a low defense for streptococcal infection, it had better be soon. . . If the patient is in another group with a very high defense and not much danger of overloads, and if it is a tooth that is greatly needed by that patient, I would advise you to do what I do: retain some of those root filled teeth, because I believe they are of more value to the patient in the mouth than out.”2
Price’s counsel, delivered during a 1926 dental conference, still holds the weight of truth today. That is, most biological dentists and practitioners find that if a patient is in excellent health, he or she can handle the stress of a root canal tooth. However, it is important for this tooth, as well as any associated ipsilateral disturbed fields in the body, to be monitored over time. If at any point positive signs and symptoms arise, and the patient’s health is compromised, then the decision as to whether the root canal tooth should be extracted must be reevaluated.
In contrast, if a patient has suffered from chronically ill health for many years, then the decision of whether to extract a devitalized or root canal tooth is clearer. In these cases surgery is typically very appropriate. Or, for example, if a patient receives a grave diagnosis such as breast cancer, it is important that all root canal teeth anywhere in the mouth—but especially ipsilateral to the breast—be cleared in the face of this serious disease in order to try to save the patient (Figure 3).

Figure 3
However, even when it’s clear that a tooth can’t be saved, simple extractions can be as irresponsible and ineffective as when an untrained conventional dentist removes mercury amalgam fillings. What is required is a knowledgeable and skillful dentist and sufficient pre- and post-surgery treatment in a well-prepared patient. This type of surgery is termed “cavitation surgery.”
HISTORY OF CAVITATION SURGERY
Cavitation has a dual meaning. As previously described, a cavitation is a cavity or hole of infection in a bone. In surgical nomenclature however, cavitation surgery is the term for the dental surgical procedure that removes diseased bone from within this cavity so that new healthy bone can grow back.
G.V. Black, DDS, MD (1836-1915), known as the “Father of Cavitation Surgery,” treated many of these areas of chronic osteitis (bone inflammation) at the turn of the twentieth century. In his two-volume opus entitled Work on Operative Dentistry, Dr. Black characterized these cavitations in the jawbone as a progressive “death of bone” which was able to “soften the bone, often hollowing out the cancellous portions of large areas of bony tissue.”3 As described previously however, Black was amazed that even the larger jawbone cavitation areas full of necrotic (dead) debris could cause no visible redness, swelling or increase in patients’ temperature. However, when these bone cavitation lesions were “opened freely and every particle of softened bone removed until good sound bone forms…,” Black found that “. . . generally, the case makes a good recovery.”4 Thus, Dr. Black identified the serious pathological processes that are generated in infected teeth and bone, noted that these chronic dental focal infections were often relatively silent, and pioneered the cavitation surgery methods that are still being emulated today by trained biological dentists in the removal of these dental focal infections.
CHOOSING A BIOLOGICAL DENTIST
Biological dentists who specialize in cavitation surgery attend continuing education courses to learn how to most expertly extract devitalized teeth, as well as how to effectively clean out extraction sites that harbor infection from previously incorrectly extracted teeth. The primary cause of these jawbone cavitations in extraction sites is the failure of the conventional dentist or oral surgeon to remove all of the periodontal ligaments when pulling a tooth. These remaining periodontal ligament pieces later act as a barrier to the creation of new blood vessels and, therefore, to the regrowth of new bone. Dr. Hal Huggins likens the severity of this dental omission to the failure of removing the placenta (afterbirth) after delivering a baby: “Bone cells will naturally grow to connect with other bone cells after tooth removal—providing they can communicate with each other. If the periodontal ligament is left in the socket, however, bone cells look out and see the ligament, so they do not attempt to ‘heal’ by growing to find other bone cells.”5
In these incomplete extractions, approximately two to three millimeters of bone will superficially grow over the socket area, but beneath the bone a hole, or cavitation, will remain (Figure 4). As described previously, the term for the degeneration of bone in these cavitation areas, osteonecrosis, is defined as the death of tissue due to poor blood supply. Synonyms of osteonecrosis are inflammatory liquefaction, and, more familiarly, gangrene. Although this latter term may seem exaggerated since it conjures up ghastly images of partial amputations on the battlefield, for those of us who have witnessed a biological dentist spooning out oily black mushy bone from an osteonecrotic cavitation site, the term seems perfectly appropriate (Figure 5). Many dentists have this diseased tooth and bone tissues analyzed through pathology labs (contact Dr. Jerry Bouquot at (713) 500-4420, or jerry.bouquot@uth.tmc.edu). In one clinical study of thirty-eight patients referred by me to Dr. Russ Borneman for cavitation surgery, one hundred percent showed positive histological (tissue-related) signs of ischemic osteonecrosis (bone death) and osteomyelitis (bone marrow infection), thus confirming the clear pathological tissue within these dental focal infections.6
 Figure 4
Figure 4
It is essential to choose a well-trained and skillful dentist or oral surgeon to treat these ischemic cavitation sites. The best referral comes from your holistic doctor or practitioner if he or she is knowledgeable about dental focal infections. Referral from a family member, friend, or work colleague who has had success with a particular biological dentist can also be valuable. Additionally, going to the websites of the three major biological dental organizations in the U.S. can help further narrow down the decision-making process of choosing the right professional for this very specialized surgery. These organizations are: the International Academy of Biological Dentistry and Medicine (www.iabdm.org); the International Academy of Oral Medicine and Toxiciology (www.iaomt.org); and the Holistic Dental Association (www.holisticdental.org). Also check the Hal Huggins website (www.hugginsappliedhealing.com)
PRE- AND POST-SURGICAL PROTOCOL
Every biological dentist or oral surgeon has suggested procedures to follow before and after surgery. The following protocol is based on my experience over the past two decades preparing patients for surgery and treating them afterwards, and I hope can add to and support the biological dentist’s directions. With this protocol, along with carefully diagnosing for whom, as well as when, cavitation surgery is appropriate, and most important, the skill of a well-trained dentist or oral surgeon, I have had a ninety-nine percent success record since 1996.
PRE-CAVITATION CONSIDERATIONS
In the majority of cases it is best to clear the mouth of heavy metals before cavitation surgery. In fact, this may even obviate surgery in some individuals who have galvanic-induced dental foci as described previously. Additionally, patients with non-toxic dental restorations heal much better from surgery than those with toxic metals in their mouth. In contrast however, mercury removal is often contraindicated in cancer patients (until the tumors are cleared and lab tests negative), whereas cavitation surgery to remove the root canals and other devitalized teeth can be clearly indicated, tolerated well, and even life-saving in this population of patients.
It is also important that liver detoxification pathways and kidney clearance functions are as optimal as possible. A simple Comprehensive Wellness Profile (CWP) from Direct Labs (www.directlabs.com) is a very affordable (over $500 worth of tests for only $97) and easy blood test to run to determine the functioning of these, as well as other organs and systems, in the body. Of course, a complete history and exam should also be performed by the holistic doctor or practitioner and the biological dentist to further assist in making the decision if the patient is healthy enough to undergo dental surgery.
If an individual is very ill, it is often necessary to have this patient on his or her deepest homeopathic constitutional remedy for at least a month or two in advance, in order to facilitate immune, metabolic, and nervous system functioning before surgery. The new Sankaran sensation method of constitutional homeopathy is the single most curative modality known by this author to achieve health, and thus prepare an individual for a successful surgical outcome.
Another important assessment to make before surgery is to determine whether the patient has a major tonsil focus. Chronic tonsil focal infections and chronic dental focal infections feed into each other and further infect each other. Patients with a chronic tonsil focus who want to have their wisdom tooth cavitation sites treated, for example, often don’t heal well. This observation was made in the 1920s by Dr. Henry Cotton (1876-1933), a brilliant, if controversial, psychiatrist who specialized in researching the effect of focal infections in the onset of mental illness. In his book, The Defective, Delinquent, and Insane, Cotton asserted that in most cases the wisdom teeth were not infected because they were impacted but were impacted because they were infected, and that this “infection is transmitted from the tonsils.”7 Before these suspected primary tonsil focus patients have dental surgery therefore, it is important to reduce the tonsil focus through avoiding commercial pasteurized dairy (the typical allergy food that causes chronic upper respiratory infections and the tonsillitis in childhood that eventually coalesces to a more hidden chronic tonsil focal infection later in life), rubbing Notatum 4X drops over the tonsils on the upper anterior neck area, and to be on their constitutional homeopathic remedy according to the new Sankaran system.
Finally, vegans, and even many lacto-ovovegetarians typically do not consume enough protein to heal tissue, and thus, the surgical site, adequately. Lacto-ovo-vegetarians often become sensitive to the over-ingestion of eggs and dairy foods over the years, which greatly reduces their absorption of these normally utilizable protein foods. Lab tests and energetic testing can determine if a patient is deficient in protein, and if so, the encouragement of eating more eggs and dairy (if there is no allergy) as well as meat broths if the patient is willing, is often needed for at least one to two months in order to have a successful surgical outcome.
THE FIVE HEALING DAYS
It is imperative for patients to take at least three days off after surgery, but the most optimal protocol is to take the day of, plus the following four days off, a time period I have labeled as the “Five Cavitation Surgery Healing Days.” Patients should plan to rest and avoid any strenuous physical activity during this time. In fact, any exercise (except slow and short walks) or vibration from extensive car and plane travel can delay, and even block, healing of the surgery site.
This rest and healing time is significant because if a “dry socket” forms from the invasion of bacteria in the area between the blood clot and the bone and the blood clot is lost, the surgery almost always must be redone at some later point. Dry socket is signaled by significant pain in the surgical site or the ipsilateral ear, and typically a foul odor. The standard treatment of antibiotics often does little because there is no blood flow in the area, and eugenol from the oil of cloves may actually further impair healing of the site. I typically recommend more Notatum 4X drops and laser treatments, as well as a castor oil pack on the suspected disturbed field (stomach, small intestine, liver, etc.) in the body. The best course of action though is for patients to take five full days off and follow this protocol carefully in order to allow complete healing of the site, and therefore only have to undergo this cavitation surgery procedure once.
 |
 |
Figure 5 – Necrotic bone on left, healthy bone on right.
The use of a therapeutic laser (830 nanometers and 100 milliwatts) is so effective during these five days in healing the inflamed nerves and soft (gums) and hard (bone) tissues, that it has become a sine qua non in my post-surgical protocol (available from jarek.mfg@shaw.ca). Patients rent this laser so they can use it in the comfort of their own home, treating the surgical site for one minute at a time, anywhere from six to ten times a day. This laser is so healing to tissue that it often obviates the need for any pain medication, or at the least, considerably reduces the amount of pain pills needed.
Isopathic drops such as Notatum 4x and Aspergillus 4x (www.bioresource.com) are especially helpful post-surgically to augment healing in the site. Further, they can be dropped onto the surgical site at a protocol of two to three drops, three times a day during these five days, and then one or two times a day for one week afterward. When the laser is next applied over the site, these isopathic drops are then photophoretically driven into the surgical site for even deeper healing.
Acute homeopathic remedies are also an important component in this protocol. Arnica montana 30C is most commonly prescribed to reduce pain and heal the bruising post-surgery at a dose of two pellets, three times a day, for five days, and then once a week thereafter. If the surgery was very deep and there is a chance that the maxillary (upper jaw) or mandibular (lower jaw) trigeminal nerve was injured, Hypericum perforatum 30C should also be taken at a different time of the day, but at a similar dosage schedule as the Arnica. If the surgery was particularly extensive and intense, patients may want to take the stronger 200C potency of both of these remedies. However, for those individuals who are already on their constitutional homeopathic remedy, usually redosing this remedy one to two times after surgery is all that is required.
One to two vials of the mineral-rich Quinton Marine Sea Plasma (www.originalquinton.com) taken daily after surgery further ensures healing of the gums, jawbone, and neighboring teeth during these five days. Patients should hold the contents of each vial in the mouth for approximately a minute or more before swallowing.
Finally, nutrient-dense bone broths are essential during these five recovery days. A clear broth from grass-fed organic beef, chicken, turkey, lamb, or from wild fish is especially important the first two days when the surgical incision has not fully closed and you don’t want any food particles to get lodged in there. Later you can purée vegetables (carrots, squash, turnips, onions, kale, etc.) to make a thicker soup to stave off hunger and supply more needed vitamins and antioxidants for further healing of tissues.
POST-SURGERY OFFICE VISIT
Besides the post-surgery dental visit to check on healing of the site and to remove any stitches, it is important for the patient to also see a doctor or practitioner knowledgeable in focal infections. At that visit the surgical site is checked, any neighboring autonomic ganglia (groups of nerve areas that can hold bacteria and other toxins transported from nearby ipsilateral dental foci) are treated, and any related disturbed fields caused by the focal tooth (or extraction site) are addressed if necessary. This clean up of all the areas in the body disturbed or infiltrated by infection from the chronic focal infection ensures more complete healing of the site, with no reflex “back flow,” or re-introduction of toxins or microbes, back into the dental focal area.
CONCLUSION
It is important that the decision whether to sacrifice a tooth or repeat surgery of an incompletely extracted site be made by the team of a doctor or practitioner knowledgeable about focal infections, a skillful and experienced biological dentist, and an informed patient. Appropriate pre- and post-surgery protocols can ensure a successful outcome and complete healing of the surgical site. For more information on diagnosing and treating dental focal infections please refer to my book, Radical Medicine (www.radicalmedicine.com).
REFERENCES
1. J. Bouquot, In Review of NICO (Neuralgia-Inducing Cavitational Osteonecrosis), G. V. Black’s Forgotten Disease, 3rd ed. (Morgantown, WV: The Maxillofacial Center, 1995, p.3.
2. A. Nichols, The Virulence and Classification of Streptococci Isolated from Apical Infections,” The Journal of the American Dental Association, 13 (1926), p. 1227.
3. A. Black, G. V. Black’s Work on Operative Dentistry, vol. 1 (Chicago: Medico-Dental Publishing Company, 1936), p. 4.
4. Ibid.
5. H. Huggins, It’s All in Your Head (Garden City Park, NY: Avery Publishing Group, Inc., 1993), p. 46.
6. R. Borneman and L. Williams. “Histological Signs of Dental Ischemic Necrosis and Oteomyelitis Correlated with Clinical and Kinesiological Testing Indicators” (unpublished research findings from the Head and Neck Diagnostics of America Laboratory, Seattle, 1995-96).
7. H. Cotton, The Defective, Delinquent, and Insane (New York: Arno Press, 1980 [orig. pub. 1921]), p. 46.
This article appeared in Wise Traditions in Food, Farming and the Healing Arts, the quarterly journal of the Weston A. Price Foundation, Winter 2011.
🖨️ Print post

root canal problem in my teeth
last one before my teeth create root canal problem.it have been very painful me. so you give me solution. Thanks SAROJ KUMAR
THANK YOU!
BRILLIANT, LIFESAVING INFORMATION.
NOW, CAN ANYONE RECOMMEND THE BEST BIO DENTIST IN NYC?
I HAVE AN INFECTED ROOT CANAL IVE BEEN IGNORING. NOW IM IN PAIN.
FRIGHTENED AND DESPERATE FOR THE RIGHT KIND OF HELP.
DONT TRUST MY LIFELONG DENTIST ANYMORE. HIS WAYS ARE OLD FASHIONED AND TOXIC.
HOPING TO HEAR FROM SOMEONE, ANYONE!
THANKSsmilies/cry.gifsmilies/cry.gif
Shenzi call Blanche Grube in Scranton Pa.
She is no longer recommended as she has abandonned patients who have had post operative complications
What do you mean by that? I was planning on seeing her… have you seen her or know people that have?
https://www.rejuvdentist.com/ Dr Gerry Curatola. My son had his cavitaion surgery done there and was very happy with the results.
Thanks for the recommendation. I have A consult with him next week. Do you mind telling me how much the surgery was?
Dentistry has the biggest hole in it, it is so frustrating to see dentist after dentist and get an MRI , and state of the art 3-D cone beam, a micro-magnification scan and they say nothing is wrong. They refer you to ENT and then you see five of those pricey guys then they say well maybe it is dental…then you go to the dentist. You are embarking on the epic nut journey ! Finally you are at a cavitation surgery dentist opens up the sites over the course of eight months. He has some sort of tool that determines which site is the most infected and open the sites in that order. Only to find out his tool was inaccurate and opens the most infected site last. He finds a big wad of gauze with huge infection is in there, and not only that the infection has spread to the tooth next door. And says, ” You must have one hell of an immune system” All the while you have been so sick you’ve been having an out of body experience at times! Well, for that to be determined that takes another MRI , and five different dentist until one of the dentists blows up the x-ray and says ” oh… hmmm okay an abscess is starting here” The testing method is not advanced enough … they need to the assistance of military technology maybe one of their breadcrumbs …. seriously to develop something should be able to diagnosis an infection even at 10% . I think 30% to 50% infection to be present in order for detection seems outrageous
have you had any success? Your story sounds like mine….going in circles from one doctor/dentist and test to another, and another, and another……and no solutions….still feel like hell, but now broke because of all the money spent trying to get well.
Measuring the cavitation point using EAV technology as you see in the film ROOT CAUSE, will assure you that the cavitation has been cleared. The Biontology device called the “CHIREN” from Europe can measure this point easily as well as neutralizing any bacteria or toxins that show up using the Chiren, with biophoton light remedies.. non- invasive and at the speed of light!
Hi Sandra, are you saying the chiren machine can sort out the bacteria in cavitations fully non-invasively, removing the need for surgery?
I can somewhat relate, and I’m SO sorry🥺
Biggest thing I’ve learned through the dental nightmare is every dentist has different degrees of knowledge and expertise.
And the cost is ultimately the hardest part, each dentist charges different prices, some insanely high. So IF you do find one that seems to know what he’s doing in a certain area, that dentist many times takes advantage of that by charging triple.
Wouldn’t it be wonderful to find a dentist or group of dentists with the right knowledge that would band together to form honest, ethical, knowledgeable partners, to be placed in several parts of each state?
Cavitation removal side effects
I had two cavitations removed but my health has deteriorated somewhat. I have less energy mostly. Is there an explanation for this?
You are most likely detoxing after the removal of necrotic bone/materials at the cavitation sites. It sometimes takes quite a while (months) to fully detox. These toxins have been building up for who knows how long and after the source(s) have been removed the body goes into overdrive to shed the residual, and that sometimes requires time for cleansing. Also,you may have other sites that need to be cleaned up as well.
Nobody talks about implants . What if (like me) a dentist had to remove your front teeth and now you have implants there ? Are those still causing heavy metal issues and making me sick ? Can’t very well go along without my front teeth . I have other teeth that were also cracked and we saved them with root canals . Pulling them would have meant movement of other teeth and jaw and made it impossible to eat (unless I got implants for all of them ) . I know yanking teeth and doing root canals is bad for your health but for some of us , we weren’t given any other options so what to do now ?
What about partials? My mom & have those.
My biological dentist does ceramic implants as opposed to the normal titanium implants. Maybe you could do some implants and some bridges?
This is what I learned from my cavitation surgery… I learned a valuable lesson
First cavitation- dentist was great, but he failed to put me on antibiotics or IV’s. A major infection was removed I had bunch of gauze that was left in my wisdom tooth extraction site, about 15 years prior. Anyhow, I was so sick after the infection was removed I ended up in the ER as usual total waste of money, time and energy and ended up seeing urologist that is where the infection got seated, bladder got scoped! My MD told me , the cause was obvious a huge infection was released into my body with no strong defense. All of this suffering could of been eliminated if measures were taken from the beginning.
Second cavitation, I had I decided on biological dentist that was closer, still having to go another state. He had me take several vitamin C IV’s prior to surgery stop 24 hours before surgery and then a few after surgery. No issues at all, smooth sailing. Apparently, taking liposomal vitamin C every hour could be the equivalent, and if the stomach becomes upset take aloe vera juice with it. Wishing All Good Health!
Faith can you share who you saw to the 2nd cavitation?
EcoNugenics Pectin-C (EcoNugenics.com) detoxifies heavy metals from your body w/o complicated methodology. Read thru their website to see which product you prefer — powder mixed with water or capsules. There is no die off from the detoxification process and it’s safe for children and the elderly. I gave it to my mom when she was 90 yrs old. Whichever protocol you choose, take for 3 months and I guarantee you’ll start to feel better (if indeed your problem is a high heavy metal burden). But I would try this first before going to a dr — it’s cheaper and you get the satisfaction of managing your health yourself instead of putting your health at the hands of a dr. not trained in functional medicine. There is a website for functional medicine where you can look up drs and perhaps dentists, google it. We have a biological dentist in Pinellas Park, FL (Dr. Carlo Litano, 727-300-0044). Good luck.
question
I also need to know how to find the best bio dentist in the NYC area. Please if u have any suggestions, I would really appreciate any info. Thank you
Have you found one yet?
I am looking for a bio Dentist who has a Cavitat & experience in cavitations close to MA ( except dr. Evans @ Groton Dental ). Is having a bone graft in after the removal of RC and the legament ( not sure if it was done properly) a danger in case if there’s a jaw bone infection??
Please reply to my email:
imgolda@yahoo.com
Thanks!
https://www.ifm.org/find-a-practitioner/ — may be able to help.
Dr Leonard Fazio is amazing all around.
I have 2 devitalized teeth I want removed. Please tell me the exact procedure so that I may find a dental surgeon who will perform the extraction properly. I live in Italy so I will have to find a capable dentist on my own. I should very much like any advice you could offer. Thank you immensely. Richard Costanzo
hi i live in Italy too, write me to my email address if you can, i have a lot to say, we can speak in Italian if you do. Have a good evening
rosrobb@yahoo.it
I had a root canal done a week ago, on the bottom left molar next to the wisdom tooth. I have been in pain and taking pain killer, after calling the dentist he ordered antibiotic amoxicilian 500 mg every 6 hours. I am still in pain after being on the medicine for 2 days. After reading about the deadly affects of the root canal, I feel like having this extracted, but am scared for the tooth is still very painful since the day of the root canal. Please somebody, anybody that knows what I should do, post me your reply…I am very grateful….thank you, or call me Oh, there are no bio dentist where I live, what should I do? Thank you for replying, 684 699-2839
Root canals can be killers!!! I know–I use to have three, and they nearly killed me!!! They must be extracted, but by a trained expert. The bone will need debriding so proper healing can take place. Go to this website:http://www.hugginsappliedhealing.com/root-canals-toxic.php and see if you can get a referral. You may have to travel some distance, but for your health, it is well worth it. Dr. Huggins removed my cavitations years ago with great success! You can contact me at: dotme@hotmail.com and I will assist you to find the proper professional. Good luck.
Hi Patrick please do you know of a good BioDentistry in AZ specialized in cavitations. I have many root canals.
Thank you!!
https://www.ifm.org/find-a-practitioner/ — they may be able to help you find one
I’m considering removal of a root canal tooth, and four cavitations from wisdom teeth. The dentist/surgeon I consulted recommended the following: vitamin C IV during surgery, pre and post massage, hypobaric oxygen treatment for three days afterward, and IV conscious sedation. Do you think these things are necessary for treatment/healing? (Some of them are costly.) What other things should I be aware of that I need to request or say no to?
Thank you!
Sounds like this dentist knows what he/she is doing! If no Ozone is available, the hyperbaric oxygen is next best (though more expensive)
Who was your dentist?
Hi, I just came across your post. Did you get a response to get a name for a proper holistic/biological dentist? I have a name for you who does ALL the right things. Dr Stuart Nunnally in Marble Falls ,TX. I’m having 4 cavitations addressed in the 17th of April. He was just on the Holistic Oral care Summit.
Best wishes and feel free to contact me.
How did your oral surgery go? I am in Michigan and have been listening to Jonathan ? Oral Summitnrhat someone loaned me from a few years ago. After listening to it I have to do something. I have 8 root canals and crowns over mercury filled teeth. I do not want to make a mistake and have an oral surgeon or dentist make matters worse. I do not know what to do ornwhonto go to. Can you share how you are doing? My email is dpyoung@tds.net
Hello, I am in Michigan also. Did you find a Dentist nearby? And How did everything go?
Thanks
Hi Karen!
How did it go? How’s your health, and how was surgery, etc? I hope you’re feeling HEALTHY!
looking for a dentist in Hawaii, Maui if possible, who has a cavit scanner and can clean out my sons possible gum infection. 808-870-4706 Ken
https://www.ifm.org/find-a-practitioner/ — may be able to help you
How can one stop periodontal disease and stop save bone loss?
Jaw bone infections known as osteomyelitis can make you very, very I’ll and can be fatal according to my dentist. I was sick totally dejbilitated with a mystery illness my symptoms were dizziness shortness of breath wheezing, tremors, heart papitations, rash weakness, blurred vision stiff neck weight loss total brain fog,nausea Dry heaves exhaustion. Light and sound sensitive I was sick for 2 years 8 months I had x-rays, MRI of my head, neck , and shoulders, I had digital panoramic micro-magnification x-ray, I had thermagry. I was checked by 45 medical doctors 3 dentist 3 ent octors and 3 oral pathologists we flew out of the country for immune boast, and to see if they could figure it out nothung,finally we got smart and hired a cavitation expert to open up every extraction site the cavitation expert found a bunch of gauze in my wisdom tooth extraction site and a huge infection the bone was black and when he tried to grind the bone it shattered. The doctor goes you must have one heck of an immune system…i honestly have to believe my life was hanging by a thread. It was the grace of God that we had the information we needed to take action, do research and be able to pay for it
Faith,
How have you been feeling since the the cavitation surgery and how painful was the recovery? Where did you find your expert and could get insurance to pay for any of it?
Thank You!!
Faith,
I have suffered with constant vertigo after 3 teeth extractions. I believe from how I feel and what I’ve seen on my Nuclear scans that I have cavitations with bacteria on them, but I’m in Alaska. Nobody has heard of this. They are trying to send me to a normal oral surgeon, but I feel it’s not the right choice. If you could email me with any advice as to what helped you and where you went, I would owe you the world. I have two small kiddos and no life, and I hate that they have to watch me in such misery.
God Bless,
Angela
angmann09@gmail.com
Call me for a free 15 min chat. This is the kind of consulting I do.
I have grinded most of my teeth (1/2 fake) down to what looks like my dentin layer (but only have a little pain on 2 of the lower, middle ones every so often if I chew just right on them). My dentist who is more nutritionally oriented than most, has recently recommended some possible sealants, crowns on most if not all of them, some dental implants & possibly bone transplants in the implant areas…but also muscle tested me a year or 2 ago & said I wasnt a candidate for implants. I have 1 bridge left in my mouth (the other 2 came out in the last 5 years becuz I cut back on all the supplements I was taking & the teeth under them developed caivities, etc). I have not done anything 2 replace the gaps, other than a partial denture. I also have osteoporosis (but this has improved this year since my son started helping me w/my health problems)& TMJ doesnt seem 2 cause me any pain except some neck pain which isnt constant. I am a female, 62 yrs old & have an adult quadraplegic daughter that lives @ home w/my husband & son so I have 2 take that into any decision I’d make. I’m hopeing the remineralization & Cure Tooth Decay protocols I’ve started a few months ago & prayers 4 a miracle will happen & I wont have 2 spend a lot of time/discomfort or get a lot of dental work done. (I’d like 2 enjoy our 2 precious grandchildren & life more!). Any advice u can give will help. thank you so much & God bless you.
Can l call u
I feel much better. I had a couple vitamin C IV’s after surgery, My ND put me on a few months of ozone IV’s after cavitation surgery, with amazing results.
The dentist was amazing, gentle kind, but he is no longer taking patients! There is no pain to speak of because of Centrifuge . But the recovery took about two weeks, until I felt I could really open my mouth and chew. I had lots of broth/ puree type of soups, smoothies with mega- vitamin powder mix and Kefir.
The cost for cavitation each site between $900-1200 depending on the dentist, and the labs used for analysis. I paid out of pocket some sites were done twice! I think you need to check with your insurance.
If cost is an issue, for cavitation surgery. Well there are options, a friend of mine from Asia, did not want to wait for Visa to travel here. So he went to the dental clinic for dental cavitation where Dr. Villafana in the in Toremol building, in Tijuana he felt the surgery was successful . Many Americans go to Grand Lux Hotel in Tijuana for dental work. The cost is a lot lower.
National
Top three
Dr. Margolis Mesa, Arizona
Dr. Shankland Westerville, Ohio o
Dr. Grube Pennsylvania
Dr Panapour – Bellevue, Washington
Dr Mark Breiner in Connecticut
Dr James M. Heltzel, DMD in Las Vegas ( Studied w/Hal Huggins)
Recovery is long, I’m 90% better Insurance did not pay for any of it. It is costly. Also to accelerate my healing, I did oil pulling with coconut oil with couple drops of wild oregano oil, peppermint and one drop of rosemary oil daily 30 minutes a day.
I saw Dr. Panapour in Bellevue, Wash. I had to travel about a nine hour trip. If you book have your teeth cleaned before you arrive. First appointment he examined me and sent me home! Then I booked again for some of the work . Total of five trips for it all get done. It is best to find someone close by. Where are all the dentist who do this work hiding?
Most holistic dentist say there is no way to cure bone infection unless you go in and clean it . Medical doctors give you antibiotics IV for bone infection.
Many holistic dentist suggest ozone injections at the site
of infection. I hate the way ozone makes my brain feel. Laser is supposed to be best, I haven’t tried it but have heard good things about it.
Since my jaw still aches sometimes I know there is still some
thing going on. This is what I do I’m not saying you should this I’m just telling my story. I did research and decided to come up with something to help me. I have been doing this I mix MMS three drops in 1/4 C of water with 1/2 tsp DMSO and I put in my mouth and hold in the area infected for five minutes then I SPIT it out in the sink. I also hold a near infrared light and shine it on my jaw daily for 10 to 15 minutes
After this work my ND suggested Ozone, intravenous drip so I agreed and I had that for a couple months . My MD was not to thrilled with it, My ND was thrilled with it. I felt incredible and I think it really helped kill any other little infections.
Dr. Oksana Sawiak appears to know a lot about this
issue and I really love this site it really explains a lot and the illustrations are good.
thank you for the information in have surgery next week in colorado .if it does not work i will call the drs you talked about
I’m in Colorado and would like to know who you used and how it turned out?
wandalou@comcast.net
Hi, I had cavitation surgery, and I feel horrible four years later-similar symptoms.
Can you please recommend your cavitation specialist?
HeatherLomaxMusic@gmail.com
🙏🏽
It appears any dentist (or even some non dentist MDs) can join IAOMT, so there is no standard for approving their listed dentists. Here is the link to apply online http://iaomt.org/become-a-member/apply-online/. HDA and IADBM also offer a similar online membership with no criteria, although IADBM does offer a certification program. While they all offer conferences and training, one does not need to attend these. How do you find dentists who are genuinely qualified in this field?
I discovered this too. I then poked around the DAMS website, and have only started asking some questions there. I think they may also refer to that list.
I think at this point – I just need to look up biological dentists, and then research reviews etc. myself and go for it. I need a ton of work done… I am hoping I can do extractions at a regular dentist (covered by insurance), and then some restorative work at bio (often not covered).
With all the bad news about root canals, and such, it seems there is NOTHING good to be done [post extraction! I am looking into all ceramic implants and/or bone grafting at least to keep structure of bone for back molar sites. But -again, bunch of bad news there. This is incredibly daunting.
Ozone and proper supplementation with Zirconium implants is a good way to go.
IAOMT accredits their dentist is with an exam. Those dentists can use the designation AIAOMT which meanS accredited by the IAOMT. The higher designation is FIAOMT whicheans a Fellowship has been awarded for further excellence and proficiency in the field of Biological dentistry. Yes there are various disciplines among the membership of IAOMT including MD, ND< Chiropractors, Lawyers, Hygienist, Activists and Authors. anyone who stands for Science in Dentistry is welcome as an associate member or as a friend of the organization.
I head this from my dentist that he did not want to pay
8000 to have his name on the holistic dentist list I forgot the name of site I was stunned that you would have to pay for something should just be given it is professional and ethical obligation
please tell me how to get a diagnosis for jaw cavitations
The least invasive one is a Cavitat scan (like an ultrasound of bone) We have an instruent in our office.
I had 2 teeth pulled in September and my gum still will not heal and the pain is unbearable. My oral surgeon did a panoramic x ray yesterday and said it just needs more time to heal. I can’t bear the pain anymore. Can you tell me where the is a dr that can help me please?
you are like me i g0t teeth pulled a month ago. an it does not close up or heal and the x rays does not show soft tissue infection .you need surgery and find a cavitat scan .look at faith words on this page.for the right dentist. i went to a half dozen dentist many xrays they all say no infection. its the wrong x ray .i get this funny taste in my mouth. yesterday i had to tell my oral surgeon.that im 110 persent that i have an infection.so shes going to do an explore surgery .if she finds infection she will go deeper and clean it out.do not give up keep reseashing ,and searching for a dentist to beleave in you. i have been fighting gum infections for 5 years now off an on i have had 8 surgeries so now i educate my self an make many phone calls.
Would it be beneficial to see a chiropractor or acupuncturist the day after having a tooth extracted. I had a root canal about a decade ago which has since cracked, chipped and left me with an infection. Or should I try to make an appointment with a chirp or acu a week latere after the five day healing time? Also if I can only budget in one holistic practitioner which would be more beneficial for healing of the jaw an acupuncture session or s chiropractor?
Aside from bone broth what is recommended for the first two days? Is geletain in warm water suitable substitute if i run out of bone broth? I was planning on sliced steamed pieces of whole veggies and pastured meat that I can swallow without chewing. Is raw milk and raw eggs out for those two days? Or should I avoid things like that for longer?
Thanks
I would recommend the eggs for sppedy healing. If there is any dairy intolerance at all wait with the milk. Also enzymes from Papaya (papain), pineapple (bromelain) and vitamin C D3 and K2 are all helpful in getting the bone to heal faster.
Juicing and smoothies would be good. I would go with an acupuncturist and then a chiropractor in this case. Powdered collagen is also good for your connective tissues and bone health.
I had a slightly infected 20 year old root canal removed 5 weeks ago. I am so exhausted I do not know what to do. My immune system is fighting off the infection so hard that I can hardly get out of bed. I do not have any symptoms other than exhaustion and a very dull ache where the tooth was pulled out. It was my top back molar. I know if I go to the doctor they will put me on antibiotics. You say here in your article that these infections are so deep that antibiotics will not help. Please help me with some guidance of what I can do. thank you
Depending where the tooth was, sometimes Ozone and Rife will take care of the infection without exposing you to the need for antibiotics which may not do the trick in the first place.
Blessings
Hi terri, hope you are well, I had a lower molar extracted 4 weeks ago due to decay and absess, it all started years ago when a filing fell out if the tooth and I did not go to dentist as had a bad exprrience when younger, in august this year one night I woke up sweating , heart racing, felt sick it woke me up bigtime I didnt think nothing if it at first then hapoened again, this is when I noticed I had a small absess and it was hurting, I took the courage to vusit dentist who prescribed amoxcilen this did not clear it and had to go back for metronidozole these also did not clear it, I went back a third time and was given something begining with c, then I had to wait 5 weeks to gi back to dentist to have the tooth extracted, the absess was still there not a big absess but still there, now 3-4 weeks after I have similer symtoms of when I first found the absess, waking through night sweating, heart feels like missing a beat, tender tummy, feel sick kinda like flu symptoms, is this normal, I have been to d
Dr and tgey doing blood test, think I had absess too long befire doing anything about ut and my bidy is still fighting infection
ahy advise from anyone?
This is the kind of information we help people with. If you wish to give us a call, we can have a free 15 min chat.
Hi, I have some bed teeth and really need help with what to do!!!
Recently I learned that teeth that have not been killed by root canal can actually be repaired if the body is given the proper nutrition, good rest, exercise, non-toxic water. However, if we have had a root canal, as far as I know the tooth is now dead, and cannot be repaired. It traps the bacteria, and that bacteria (that are present in the mouth and are not normally harmful)morph into more aggressive and toxic bacteria that is difficult for the body to fight, since there is not much (if any) blood flow to that area.
I believe that God has created our bodies to heal themselves. What I am concerned about as I am considering having 3 root canal teeth removed, is that if I undergo surgery and have them remove the periodontal ligament along with infected jaw bone, that I am not allowing God’s natural healing processes to occur. I understand that me having the root canals done in the first place was interfering with God’s healing process, but I want to minimize mechanical and artificial methods from this point forward, as much as possible.
I would like to know what my options are. If I have the teeth extracted, but leave the periodontal ligaments and the jaw bone in tact, what are the consequences? Why can the jawbone not heal back if the periodontal ligament is left? Or can it heal, but might take a longer time?
Sincerely,
Air
If the ligaments are left in, the bone can’t heal ‘through’ the ligaments. The bone cells find ligaments material and stop there. So, the potential for those ligaments to cause cavitations is apparently great. I’m not an expert but I have read this a few times from Dr. sites. I am wondering though also, I need root canals extracted but … I have no idea what the right move is after that… I am sick now, and I’m worried my body isn’t up to much… but certainly want to find the best solution. Implant? Bone graft? I can’t have 8 holes… my jaw will dissolve. (Jaw bone needs blood flow and stimulation to continue growing or it resorbs. That’s why it’s important to fill the gaps with something but… but what?
Oy…
Hi! I have been diagnosed with staphylococcal infection in all four areas where my wisdom teeth were extracted. In addition, I have a cavitation problem where another tooth was extracted. The tooth was dead and it had a massive abscess that had grown into my sinuses. I was now told that the staph infection is in my sinuses too. I am with a biological dentist and was advised that, as part of the surgery, I could possibly lose 5 further teeth if the infection has spread under the bone where the teeth are held. Needless to say, I am absolutely terrified of the surgery and the thought of needing dentures at my age (I am in my forties). Any advice for me how to handle this? Also, is it absolutely necessary to remove further teeth that are currently healthy? Thank you.
I am in a similar situation. I have researched things to the hilt, but I am now in need of guidance. I have to drive a love way to a bio dentist which takes no insurance. I am hopeful I can get some extractions done at my ‘covered dentist’, but really work through the bio for any restorative work and for all the amalgam removals. THing is most of my amalgams are under crowns in root canal teeth!
I’m looking at more than 10K in work (there’s a load of debt I don’t want but I’m quite sick and need this work done… it’s taken my over 8 years to figure all this out!)
Cavitations I haven’t even figured into things -as my first priority is mercury and that is 8 teeth, 4 are root canal/crowned. BUT…I know I will have issues in jaw bone as well. I’m looking at 5+ extractions, at age 40. Implants? Partials? What do I do?
I hope some folks can reply…
I am retired from holistic dentistry and now do counseling for people in situations like yours. Call me if you wish for a free 15 min chat.
I have been in pain for 25 years. I was diagnosed with tmj in 93 and had surgery. 96 trigeminal neuralgia with microdecompression. Rhizotomy, gamma knife, and a shot in the nerve. I think I may have 2 cavitations in my mouth the pain never goes away. I have had bad thoughts and pray everyday to find a solution Thsse procedures never took the pain away. I had a root canal and an apilectomy on a bottom tooth and I lost the tooth anyway. That is the side where the pain started. By the grace of God I am here an searching for help. There is a dentist named Diane Meyers in Downers Grove Illinois and she claims to be holistic. I live in Bloomingdale Illinois.
God bless you for that.
In our clinic we use Ozone, Rife and Vitamin C to clear many of these without surgery. It depends where the infection is and how enclosed it is in cortical bone. If you wish, give me a call for a free 15 min chat.
I have read of a case on line, this girl does tons of research and just does not want cavitation surgery so
she decided on ozone to be spun/mixed with her blood and
then injected into the infected sites and she was cured.
There is medical blue laser machine that kills all pathogens my doctors office has one and you can rent it for like 125 for a week.
David:
Do you have a web link to this story — or the name of the patient or dentist involved? I have researched the web but I cannot find such a story. It sounds quite intriguing. Thank you.
Have you tried oil pulling with a few drops tea tree oil in it? It won’t taste good but it will start to disinfect the area. If not familiar with oil pulling, google it. Oil of oregano will also act as an antimicrobial. If in pain put a clove in the area where the pain is, it will numb it naturally.
I am desperate to find a good dentist in NH. I have yet to find ANY on any lists online. I have to believe there is some dentist practiced in SAFE amalgam removal and cavitation surgery. Anyone?
Have you looked at the http://WWW.IAOMT.ORG list? If you have trouble finding someone, give me a call. Perhaps I can help.
hello about 3 weeks ago I have tooth #5 removed due to a bad root canal situation…..doctor was honest and recommend extraction,this is 3 weeks later tooth # 11 has a rootcanal and tha bottom underneath feels like is inflamed and feels like root canal too ……what is all
trying to tell me…..I am 60 very healthy active lady w/lots of energy and life this is not good news for me…..don’t take any medications even stop to have a rum and coke..please hekp
This type of consulting is what I do. Check out my website at http://www.drsawiak.com and if interested, give me a call or email me.
When I do Cavitat scans, I often find cavitations on the sites that cross the meridians of the person’s symptomatic organ e.g. Breast cancers invariably have a cavitation, infection, root canal or toxic restoration on teeth #6 and #7 on the upper and #4 and #5 on the bottom jaws on the same side.
There are many procedures in addition to surgery that are useful in eliminating these debilitating infections.
A dentist lied to me. I told her I do not want a root canal just clean real good and I want a crown. One year later for a exam at UCLA I find out I have a root canal to my surprise. I had schedule extraction as recommended. Appointment for February 19th 2015. A few days later after the appointment I abscessed and asked to be on anti biotic. I was in pain and asked for it to be drained. It got drained and what a relief. Anti biotic did help but I was not well. I had a emergency appointment and I had tooth extracted on Friday January 23rd. I have pain and bad breathe. When the tooth was pulled the dentist just cleaned with water. infection was in my bone and if I wanted an implant I would need a bone graft and first I need a surgical procedure to raise my nasal cavity due to the area. It is my top left last tooth. I went again on Monday January 26th, 2015. The dentist wants me to take a stronger antibiotic. Thanks. I live in Sun Valley, Ca. Southern California. Irene 818-572-5052
Where is Dr. Oksana Sawiak and is their a phone number please, so I can call.
Will cavatation show up on a cat C.T. scan? Have Rheumatoid arthritis for 45 years. Diagnosed after extensive dental work and gum surgery. all teethe removed. later and showed extensive cavatation. Had cheek/gum sensitivity, diagnosed with x-ray tooth root remaining up by sinus wall, had it removed. now still have gum /cheek sensitivity/discomfort. also have ringing in both ears, swelling in left cheek.C.T scan results: sinus clear but fatty tissue in left cheek which shows as more fullness in left cheek. Could I still have a cavatation problem which is not showing on C.T. scan and contributing to my auto-immune problem ? Thank you, Margie
Hi I live in the UK and cant find a biological dentist that does laser treatments, Ozone therapy, nutrition, isopathic remedies etc. does anyone know of a biological dentist in the UK that does these treatments.
Hi Sophie, did you visit Munro Hall in the end? I too am in the UK and am struggling to find someone to help me with Ozone etc. I have developed an auto immune disease when a friend recently asked me if I had any teeth work done recently. I then realised that the first sympton was a tooth!!! I’m desperate to get this looked at so I can get back to a normal life and not a life trapped in bed. Thank you.
Hi Rachael, did Sophie ever get back to you?
I also am from UK , but live in Arizona USA at the moment. Can I help ?
I have much dental needs too but going to a dentist in Mexico recommended by Dr. Tennant, Tx Got a passport?
Email me we can see if there’s a solution here – Jini
Jinimurray@gmail.com
Hi
I too 2 yrs ago was diagnosed with an auto inflammatory condition left me bedridden – I’ve been in de Jak about my cavitations that I’m told I have
Be good to speak with more from the the Ik who are struggling with this
Hi Sophie,
I would contact Munro Hall in Bedford. They have a website which you can find on the net. Just type in Munro Hall.
Hi Justin thanks for the dentist recommendation I will contact them and see what other holistic or biological treatments they do apart from removal of mercury fillings. have you been there before thanks again.
Hi Sophie, have you managed to find a biological dentist in the uk? I am also looking for one that does Ozone therapy as I’m concerned possible cavitations from my wisdom teeth are causing my health problems.
I’d be grateful for any advice.
I live in America now, but have been treated by Munro Hall and they will take care of you excellently. Go Go Go. They are a blessing, as they do metal removal, IVC and nutritional supplementation so you will be back to good as new. Infection removal is total. They are thorough.
I live in Woodbridge, VA (Northern Virginia area) I really need to find a holistic/biological dentist. Can someone please help? Thanks
Dr. Fischer in Annandale (703-256-4441) or Dr. McClure in Washington (202-237-7000)
Please Help!
Does anyone know of a good dentist in the NYC area that can take a look at my root canal and other tooth problems. I have a host of symptoms including cysts/nodules. Can root canals and other tooth problems cause this?
Any information would be greatly appreciated.
Hi, I have read the above comments and would like to know what some of you have done to regain your health after your root canal removals and caviattion cleanings. I had one root canal removed and a HUGE cavatation cleaned in my lower right jaw. I go in to remove the root canal on my upper left next week. The cavatation was the largest that the Dr had seen in his 20years of dentistry. I had thermal imaging done that showed the infection. Infection from the cavatation was going to my heart. I felt really weak after the surgery and ended up in the ER with dehydration. While there they put me on an IV antibiotic and sent me home with a ten day supply, thinking that they infection from the procedure had gotten into my system. I didn’t feel any pain like I had before the surgery…..muscle, stomach, sore glands….but I was really weak. After two weeks I went in for a detox with a lady who does bio-resonance work. The detox she did was too strong. Now I feel worse than before I had the procedure. Can any of you who have been through this advise me on what you did to help. I have googled so much but to no avail. I don’t have the finances to do much more seeing that I haven’t been able to work since the procedure. The dentist who did the procedure is highly recommended in his field. He has a very good record of helping people. But he hasn’t had much advise to give me other than to find a good ND. Thank you for your help!
Wondering how you are feeling? I need cavitat work done but am very fearful….
I don’t know if you are still struggling with your health, but I had to write after reading your story. If you can’t afford lots of additional naturopathic treatment at this time, probably one of the best things you could do would be to start with liposomal vitamin C by Livon Labs. It has made a world of difference for me and is much more affordable than the IV vitamin C drips I was getting. I can literally feel it working. They say it works as well as the drips. This company makes real lipsomal form. Take a look at their website.
Who did your procedure? Also, maybe your detox pathways weren’t in peak condition. Cell Core has great products and an amazing foundational phase to help with detox organ support.
Does anyone know of a bio dentist in Texas? I have several fillings from years ago – I want them out! Two of the fillings have teeth that have broken off with exposed areas. Thanks in advance for your time…..
Kathleen, how are you now? I wouldn’t get another root canal removed until you feel strong and healthy again. Leave the bio-resonance procedures too. Have you seen a doctor? If not, go and see a good doctor and see what they advise. And pray to God to help and heal you! I hope you get better soon.
There is a great bio dentist office in Marble Falls, Texas. Dr. Nunnaly, Freeman and Owens. I had a root canal
in the upper tooth number 3 removed in August. They used iv sedation and vitamin c iv during procedure along
with accupressure following the procedure. Very impressed with the lack of swelling and pain from the extraction.
They even use your own blood to heal the site more readily. I have a question for anyone that has had trouble with
an old root canal, if they have had a rash. I had one all summer before the procedure on my neck and under
eyes and jawline. It went away after the procedure for 6 weeks and has unfortunately returned. I’ve tried everything
to get rid of it. I’m going to use vitamin c packets that they had at the dental office and probiotics to see if they
will help very frustrating to have a rash on your face for so long.
Sheri how is your health doing now? Can you pls tell me what was used in place of your extracted root canal tooth? I have an infected root canal which I first had done 15 years ago, then redone 10 years ago and I’ve recently been told there’s an infection up in the gum/bone as not all the root was treated. So I am looking to have it extracted. I need to find a biological dentist/surgeon who specialises in cavitation surgery. I’m trying to figure out what is a holistic approach to having the root canal extracted and what is used in place after? I was considering a dental implant but discovered that they also have health risks. I have had chronic health issues almost 8 years and I am now wondering if the infected root canal tooth has been playing a major part. Would really appreciate any feedback on what was used after as my understanding is that if a whole is just left then that can cause one’s teeth to grow into the gap and other problems? Thank you!
Yes, I had geographic tongue and a rash and my face looked fatter. As soon as I had the infected root canal and wisdom site extraction site from twenty years ago removed, it all was fine. Highly recommend. I sent myself to an oral surgeon as I didn’t want a dentist mucking with a knife. Besides, I my opinion of dentists and endodontists is pretty low as I’d had a total of six different practitioners tell me I was fine. I had the biological material from my mouth sent to an independent lab, I mailed it myself from Berkeley. Glad to share results when they arrive.
Can you recommend a biological dentist in Northern California?
Thank you.
Does anyone know of a biological dentist near Morgantown, WV? My son was in a bad motorcycle accident and he needs help! I don’t want him getting anymore root canals, as I had one that got very infected and cost thousands before I found a dentist (in Ellicott City, Dr. Sam at Julian Center) to remove it. He is so backed up and far away, I need to get my son into a good dentist soon. Thank you for help!
A Friend of mine saw Dr. McClure in Rockville, MD. I plan to see him about a suspected cavitation. Rockville may not really be any closer to you than Ellicott City, though.
Hi there, I wanted to just check in and see how many of you found you had cavitations on non-wisdom teeth? Can cavitations be identified via regular CT scan or does it have to be via Cone Beam Technology or Cavitat? Does anyone know of a biological dentist in Israel who knows about this all?
i started useing SANGRE DE DRAGO for my gum infections . its a sap from a tree in south america.it helps and buys me time to find the right dentist. find it at alpha omega labs
The International Academy of Biological Dentistry & Medicine – IABDM has a directory of Biological Dentists & medical professionals world wide. visit http://www.IABDM.org
My mother and I are terribly suffering from heavy dental pathologies to such a point that we now have strong heart problems as well as neurological effects as I am concerned. It is becoming a real nightmare.
We both live in France and have not been able to find a skilled practician.Briefly: 8 years ago, my mother had a cleaning of a root canal on a devitalized teeth which had to be extracted. This canal got perforated during the cleaning and almost right afterwards and since then, she had this terrible pain with strong bacterial and mycosic infection with a cyst. A last x-ray exam also show an osteonecrosis of the bone.For those 8 years, my mother has been taking- and is still taking- morphin with antibiotic and cortison to calm the pain and can barely sleep at night.
As I am concerned, I had very large amalgams with 10 extractions over those last two years besides a cleaning of one root canal 10 years ago on a premolar that finally had to be extracted 9 years ago. I have lots of foreign bodies, roots left in the all gum as seen on the last x-ray exams as well as multiple osteomyelitis. And since February last year I am experiencing terrible neurological symptoms as well as heart problems with arythmies and feel at moments like I will be losing my life. I suffer in my all face, eyes, nose and jaw. And all of this is just awful to live with everyday.
Do you ever know a bio-holistic professional doctor, dentist, stomatologist, any skilled specialist practicians- preferably in Europe as I do not see myself and neither my mother take the plane in our actual physical conditions, who would be able to heal the both of us of our heavy dental-gum and jawbone pathologies as this situation is turning really unbearable and so painful. If not, we would be open to any names you could provide us in the USA or wherever else if we do not have any solution in Europe.
You can email me at: v.degraeve@orange.fr
With many thanks in advance for your precious help.
Veronique D.
Hi Veronique,
Did you manage to find such a dentist in Europe? If yes, please respond here or email me with his/ her name and contact details. Thank you very much! Best regards, Ellyse sunset.cd (at) gmail.com
https://www.swiss-biohealth.com/en/
Hi I had an infected root canal extracted 5 days ago and I am in a lot of pain, seems to be getting worse. I haven’t had any antibiotics but just using homeopathics and high dose vitC. It’s the weekend but I will call my oral surgeon tomorrow. What should I be asking for? Him to clean the extraction site
again? Check if he removed the Periodontal ligament? Also he is planning on an implant with titanium I’ve heard that zirconium is better how do I test for comparability? The Melisa test? I’m about to resort to antibiotics as I can tolerate much more but reading through it seems it won’t do anything. Any help please.
Regiani dental is an amazing holistic dental practice in Metro Detroit (Clarkston); Dr. Regiani is not only one of the leaders in the field of holistic dentistry but also a pioneer. He truly works on total body health and would be a fantastic choice for cavitation needs if you are located anywhere around Metro Detroit. I have been going to his office for almost 30 years and he is now working with my husband to see if there is a possible link to his vision loss (retinitis pigmentosa) and potential cavitations. I will keep you all updated . . .
Hi Angela. I live near Brighton, MI and noticed your recommendation of Dr. Regiani. Didnhe help your husband regarding hisneye sight?
I am looking for someone to remove numerous root canals and crowns that are covering mercury filled teeth. I am panic stricken trying to locate someone qualified. I fear having problems from the extractions. I am new to learning about what to look for in a biological dentist and don’t trust my judgment yet. Couldnyou email me at dpyoung@tds.net in hopes of me hearing about your experience with Dr. Regiani. Thank you.
Does anyone have a dentist recommendation in the MidWest? I live in Iowa and I’m ok with driving to see someone. Feeling very dizzy, dull ache in upper front tooth that had a root canal done 15 years ago. Extreme fatigue and brain fog as well with stiff neck all on the same side as the root canal.
Hi Amy, Just wondering if you found a biological dentist and are feeling better now? I went to Dr Cody Kreigel in North Liberty, Iowa and have had amazing results after having cavitation surgery. Just hoping you were able to get some help.
I have a cavitation from a root canal that I never had filled or capped over 10 years ago. I can’t afford a cavitation clean-out surgery right now but have been doing some research.
Dr. Christopher and others successfully treated and cured gangrene by applying marshmallow root tea on the affected areas. Cavitations are very much like a slow-growing form of gangrene.
If I have the problem-tooth extracted but I do NOT use a gauze to allow a clot to form, but instead I treat the open area (which has access to the cavitation) with marshmallow root tea, do I still run the risk of developing dry socket?
If I did this, would I (like holistic oral surgeons) need to scrape away the old black dead bone?
Sine the documented treatments of curing gangrene with marshmallow root only have accounts of gangrene on limbs, and not somewhere internal such as a cavitation, it is unclear whether or not the area would heal itself or I would need to scrape away the osteonecrosis. Also, I have to take into consideration the fact that this infection has been forming for so long that the bone may have to be scraped away because my only comparison is the gangrene on limbs that healed without any scraping.
Also, since the marshmallow root tea would be very healing to the area whether I would have to scrape it or not, could the tea prevent dry socket?
I do not know how may days I would need to do this but from what I’ve read gangrene heals from marshmallow root within 2 to 3 days.
Just for clarification, I swelled up so badly this week I went to the ER for antibiotics to treat the infection in the tissues, but this does not treat the anaerobic bacteria, they are impossible to treat with antibiotics as they are not flowing in any fluid, they are just living in a pocket of space above my tooth.
After the ER, I went to the dentist who was going to attempt to extract the tooth, but I couldn’t get numb because of the amount of swelling, and so he decided to suction out as much of the infection as possible. It was the very worst pain I’ve ever had in my entire life and I never want to feel that again.
I still have the infection, I’m still swollen, I’m still on antibiotics, and I’m on a list for a dentist to extract the tooth when my swelling goes down…assuming that I would be able to get numb which I have a high tolerance for to begin with.
Any thoughts on this would be appreciated, I love learning and I’m in a severe amount of pain and simply cannot afford a cavitation surgery right now. But I am trying to save money to have a cavitation surgery and bridge/implant for that tooth done in Mexico because it costs much less there.
Thanks for reading.
Though not a healthcare professional, I have apparently relevant experience and knowledge. One, by way of Vonderplanitz’s Primal Diet, I have consumed ‘high meat’, fostering decay of my body’s degenerate tissue, rapidly replaced by healthy tissue through my consumption of fresh raw meat. (I have also, as not indicated by Vonderplanitz, consumed decaying cooked meat to similar but accelerated effect, though with unpleasant bowel distress.) Two, I have experienced pathology via jawbone cavitations. Three, besides my essay helping explain how the Primal Diet can accomplishment of such tissue regeneration [https://www.amazon.com/gp/customer-reviews/R2A0YRGVA4LROE], I am the main author of the Wikipedia article on focal infection [https://en.wikipedia.org/w/index.php?title=Focal_infection_theory&oldid=721835114].
Admittedly, I did not read your whole post, a short essay apparently seeking free healthcare counsel about your hypothetical, maverick dental tactic inspired by frugality. Anyhow, I cannot see how tooth extraction without ample socket debridement would allow clearance of a focal infection there. Unlike soft tissue of limbs, jawbones have poor blood circulation and lymphatic drainage, and so lack a simple route for decaying bone to evacuate the site. Further, sites of extraction of even healthy teeth tend to develop cavitations, to begin with, through lack of debridement of the socket to remove the soft tissue, the periodontal ligament. In any case, there is always a risk of ‘dry socket’ after a tooth extraction. Failure to plug the hole, and instead flushing it tea, seems inevitable to raise the risk of that.
A side note, I don’t suggest an implant if you have any hint of infection. I have had tons of friends who have had to have them removed.
Does anyone know of a biological dentist in Israel who knows about this all?
Sofia
Look for an oral surgeon who treats cavitations. Ask what the surgery protocol is. And read http://www.debugyourhealth.com/dental-cavitation-root-canal-infection-dental-implant-infection/ for some super useful details (I followed her surgery checklist with much success)
Looking for a biological dentist in Ghana, West Africa for a tooth extraction.
As far as I understand, to avert formation of a jawbone cavitation, a routine tooth extraction usually does not particularly call for a biological dentist, but calls simply for a dental surgeon who is willing to, and then who does, thoroughly debride the tooth socket to remove the periodontal ligament’s remnants.
I had a total of 5 cavitation surgeries. The first one was unsuccessful but the second one was successful. I finally got rid of the ringing in my ears, constantly tight shoulders/upper back, and a draining feeling down the back of my throat.
I summarized my cavitation surgery lessons learned in the following article. It includes practical tips and a printable checklist. If you decide to have cavitation surgery, these tips and lessons learned will hopefully help maximize your chance of success.
http://www.debugyourhealth.com/cavitation-surgery/
Your surgery checklist saved me!!!
What type of surgery did you choose..do you have any helpful tips or advice. Thank you
This guide is INCREDIBLE!! Thank you so much for creating and sharing!
Looking for a dentist/oral surgeon who has a holistic/biological approach to cavitation surgery in Canada?? Ideally in Alberta if possible but I’ll commute if needed, but local would be really helpful. The city I’m closest to is Calgary.
Needing to have an old root canal tooth properly assessed and then likely extracted due to infection. Have had the root canal tooth done twice – first time 15 years ago and then again 10 years ago and recently by holistic hygienist discovered on my x-rays that there appears to be an infection up there and an untreated portion of the root so I believe its best to have it extracted especially now that I know the dangers of root canals. I want to use natural remedies for treating the infection ideally not antiobiotics as I have chronic health issues and I’m not sure my immune system and gut can handle antiobiotics without further damage.
I’d also like to know what is a holistic apporoach to use in place of the removed tooth thereafter? As I’ve discovering that dental implants can cause auto-immune diseases and other health problems. Do you just leave the gap of the missing tooth or what can be used? Thanks in advance!
Evans Dental Health and Wellness 403-286-2622. Just went there today, have tooth extracted tomorrow.
Hi Tanya, I saw someone on YouTube who had great success with Dr Elmajian in Vancouver. I live in the UK but the guy who saw him (Ryan Kingsbury) said he was very good. He uses ozone, PRP and includes something for the new bone to grow on, like a sort of scaffolding. Hope this helps : )
Hi Liz
I’m looking for recommendations for bio-dentists in the UK. Lovely to see your comment!
I wonder if you could possibly help? Am also interested in laser therapy for cavitations if anyone has info on this strategy? xxx
Safe technique: ask your IAOMT dentist: NO removing teeth (except if it is already cracked) necessary, even infected if your dentist uses Endocal 10 (Albuca) for permanent cure.
No implanting necessary either.
What is Endocal 10 (Albucan)? I have a cracked tooth (top molar filled with amalgam) that is being assessed by a v reputable Endo tomorrow & am concerned about possible root canal – it is stable no pain. If amalgam is stable would best option be to leave alone at this stage?
Thank you so much for this amazing info!
i am looking to rent an 830 laser. i have an extraction on friday. i emailed jarek.mfg@shaw.ca (per above) yesterday but have not heard back. but shaw.ca now shows as a phone/cable company. does anyone know where i can rent one?
thank you!
daniel
Anyone know of a good dentist for a root canal extraction in Ontario or Canada?
Thank you
I have a wisdom tooth growing out and it keeps becoming inflamed. Everyone tells me to get the tooth removed, because it will not ever heal, they say. I do not wish to remove it. What is your advice? And how long does it normally take for a tooth to grow fully out?
I think I have a cavity. I have some sensitivity on near one of my molars. I’ve been using a clay toothpaste and coconut oil. I’ve started pip pulling again since this started. I have a relatively clean diet with some slip ups, but am getting back to it. What should I do about this? Keep eating right (paleo style) and oil pulling?? Thanks!!!
I have a wisdom tooth that has fallen sideways and is pushing into the brain stem nerve. My dentist recommended removing it as soon as possible claiming that it might be to late to remove if it gets any closer to my nerve. Do you think I should I should have this tooth removed? What about the rest of my wisdom teeth? I am 23 and do not want to suffer uneccessary treatment. I am also looking for a dentist in Minnesota if possible. Thank you for any advice or tips you can give me.
All my teeth have been out for many years and I had a cone X-ray which showed lots of cavitation in top and bottom jaw bones. Can ultrasound and light therapy on the mouth and jaw along with a healthy diet help kill cavitations? In Mexico it will cost me approximately $25000 which is less than the USA cause I have to have total upper and lower jaw opened and cleaned out. I don’t have the money My health is going down hill quickly cause of this. Please any recommendations for nutrition ect would be appreciated. Thank you
I only know of Dr. Stuart Nunnally in Marble Falls, TX. He’s an excellent biological dentist with content on Youtube. Here are examples of his material:
https://www.youtube.com/watch?v=BlFM0TmU81c&list=PLmNM4HQYBO3pxYJh_BwVKjxwrH1cYbU-2&index=39&t=3318s
https://www.youtube.com/watch?v=fV20YaQ8WSg
https://www.youtube.com/watch?v=ZxBrdDQ96HA&t=1733s
I hope that you can find someone nearby, but if not, Dr. Nunnallly and his team are excellent alternatives, they accept Carecredit. stay well.
I have filling just come off last night leaving a big hole, what should I do, one dentist suggest to extract the whole tooth out. I want to save the tooth what option do I have please help….
Rosa, we are not in a position to make a professional recommendation beyond urging you to find a biological or holistic dentist in your area.
Please email me if anyone have good suggestion for me, many thanks
Such a fabulous article! Thank you WAPF and Louisa Williams for posting!!! We are so blessed to have such incredible information about all things cavitation, and food and farming, and health and healing!!!
I have an appt. with Louisa this week over the phone; I am thrilled. She helped me in the past when no one else could. I’m happy to go to her FIRST for guidance just for me and homeopathic constitutional remedies and more.
Thank you to everyone for your comments and questions here! Today, I found out today that I have 5 infected cavitations, 4 wisdom teeth cavitations and a tooth/bone “next door.” I’m in good hands with Louisa Williams, Svetlana Yesin, Dr. Robert Jarvis, and Dr. Cowan. I am full of gratitude!! Feeling hopeful tonight. I got sick while at the Wise Traditions conference this year, made it home, and haven’t bounced back yet. I’m learning why. Support from Louisa Williams, Dr. Cowan, my incredible roommate, new friends, people inside the exhibitor area, the intuitive Tedd Koren, DC and his sweet wife, Bruce Rind and more played a role in me getting home and feeling “successful” tonight. I have something to go on. I look forward to great relief and recovery. I haven’t even looked at the papers I brought home from the conference because I’ve been managing my health challenges while back to work. I am pointing out to myself all these things “right.” Why I can celebrate… what is good about all this… so much good! So much right, especially while having problems. So much good! Many blessings!
I’m on a path of discovery, gaining understanding of my past and how it could have been guided, and healing, learning, looking forward. I will recover, and be stronger in many ways, and I look forward to helping others as my energy and vibrance come back!
Beverly
Can anyone recommend someone that is in Phoenix area that has had good results on their cavitation surgery?
Linda, did you find someone in your area? (Phoenix)
There’s Dr Nicholas Meyer in SCOTTSDALE
Email me if you like
Jinimurray@gmail.com
I only know of Dr. Stuart Nunnally in Marble Falls, TX. He’s an excellent biological dentist with content on Youtube. Here are examples of his material:
https://www.youtube.com/watch?v=BlFM0TmU81c&list=PLmNM4HQYBO3pxYJh_BwVKjxwrH1cYbU-2&index=39&t=3318s
https://www.youtube.com/watch?v=fV20YaQ8WSg
https://www.youtube.com/watch?v=ZxBrdDQ96HA&t=1733s
I hope that you can find someone nearby, but if not, Dr. Nunnallly and his team are excellent alternatives. stay well.
Can anyone recommend a good Dental surgeon that specializes in Cavitation Surgery in the Toronto, Canada Area?
How can an extremely ill and bedridden young beautiful woman who at one time was very successful and healthy now on disability and living very poor , afford to fix a diseased or bacterial ridden mouth with what she has spent all that she’s ever had on trying to perfect it . With metals and implants, root canals ,crowns and bridges, extractions and cadaver bone packed sockets ? Teeth that are what one dentist called “demineralized”. Always decaying and cracking , chipping . Now I am very very ill with autoimmune diseases and thyroid /adrenal abnormalities; early menopause that resists treatment. Complete energy loss and wakeful sleep , sweating through each night .pain all night long , pain in arms , hands , legs , ankles , neck and back problems . Very tiny narrow veins so that lab technicians can never find a vein ! The worst … being told that it’s mind over matter and I could be a productive worker and single mother if I wanted to bad enough.; because there’s nothing really wrong with me 😭
I believe that my mouth is killing me but I have no money to redo it all – or ozone therapy etc . Can you please help ??? Is there anyone who would help a person like me?
Melissa, my heart breaks for you. You sound just like me!
Only I am older. I had shocking circumstances: left me very similar to you. Email me
Jinimurray@gmail.com
Let me share with you, my hope.
Don’t give up. Never quit!!!
I have just been told that all 8 of my root canals are infected and need to be removed. The dentist wants $24,000.00 to do this with replacement of bridges on the removed teeth. I have been having headaches, and neck pain. Also I am tired most of the time, but I have always had trouble sleeping. I was a nurse who worked 12 hour night shifts for almost 20 years and retired about 8 months ago. This dentist does not have good reviews, although there are a couple that are positive. I just feel that is a lot of money for this. Not sure how to find good dentistry help? Can anyone suggest someone? I live about 300 miles from Seattle, WA.
Try participation in our facebook site NICO for further explorations
Hi, I am in Oregon and am having a similar problem. I need a root canal and have a very painful back tooth. I did a cone beam CT in April 2021 and have cavitations in all my root canal teeth and much larger ones in the jaw where my wisdom teeth were removed. I am desperate to find a dentist in Oregon or as near as possible who can help me. Any ideas who I can contact would be greatly appreciated.
Hello There,
I live in Melbourne Australia, can anyone please recommend a dentist down here? I am having so much difficulty in finding a Dentist like these good ones mentioned here. Please help 😉
There you go love:
https://iabdm.org/places/australia-1/queensland-1/margate/dentist-1/eric-davis-bds/
https://iabdm.org/places/australia-1/new-south-wales-1/sydney/dentist-1/aushi-patel-bds/
https://iabdm.org/places/australia-1/victoria-1/prahran/dentist-1/ben-olstein-bdsc/
Here’s your problem in Australia:
a Dentist [Dental Surgeon] doesn’t do anything below the Gum Line, believe it or not.
That’s the playground of the Oral Surgeon.
Good luck finding an Oral Surgeon in Australia that gives any credence to the idea of Cavitations.
The Dentists at your links are just Dentists only, so they will only be referring you to an Oral Surgeon..
I am using ozone treatment by flooding the mouth with the gas from my generator which I have been developing for several months. I am retired at the ago of 80 now with a mouthful of botched dental work. I treat the mouth twice a day for about a minute with ozone which has helped the gums very much. The upper right socket of the extracted tooth just back of the eye tooth was a abscessed root canal which was botched when it was pulled about three years ago. I am looking forward to having the socket cleaned out now because the botched extraction did not do anything but pull and say goodbye. The ozone treatment has helped the infection of that socket which was drifting up into my sinus olfactory bulb. I still cannot smell very good; but I see progress from ozone. I do not take ozone into my lungs or nose. By closing the flap in the back of my mouth the ozone enters into the mouth and exits the mouth with a Teflon plastic adaptor I made. I am an inventor therefore am able to make mechanical and electronic devices. Ozone has many good uses; but keep it out of the lungs. The ozone that is not used in the mouth goes to a bottle of olive oil where it reacts with the oil to make a good skin lotion. When not treating my mouth, the ozone goes directly to the olive oil bottle 24/7 to make the oil like butter in two weeks. I even brush my teeth with this treated oil. Much of what is in this web-site goes well with my excellent logic.
You can publish my email address as well as phone and location.
I moved to Tucson Arizona about 3 years ago for my health away from Southern California micro particle air pollution after living there for 45 years. I am a health nut like my mother; but living in the age of holistic medicine. She kept me alive when I acquired Lyme Disease back in 1947.
George J. Birds Jr.
714 E 35th st
Tucson Arizona 85713
602 531 3590
geobirds@att.net
Saw an Oral Surgeon the other day.
He says that in all but a tiny handful of cases, Cavitations are B.S..
He said that if there is an infection in a socket, there will be either redness, bleeding, a tumour, a pussy infection, or other evidence such as issues with the surrounding teeth.
Can anyone give reasons why this is not so?
Yeah right, I went through this journey with a root canal treated tooth last year. No outward signs of infection, just the pain in my head. X-ray showed that maybe there was something going there, but couldn’t be sure. After nearly a year of antibiotics, re-doing the root canal treatment, waiting and seeing… they finally cut open the gum… and found that the infection had eaten right through the bone that usually covers the root of the tooth. The surgeon was surprised that the tooth hadn’t fallen out on its own.
An infection can be festering away for many years (as it had in my case), but just hasn’t bubbled to the surface yet.
I’m getting this information too from all the uk dentists
For 2 years I’ve seen multiple dentists about my cavitations and they think it’s all BS
Due to the confusion I just focused on my overall health which was chronic – I was bedridden and diagnosed with a rare auto inflammatory disease Sappho syndrome
I refused allopathic treatment found a functional doctor – I’ve been on an array of detox protocols cleaned up my diet lost 12 kilos bought an infrared sauna went regularly to a cranio Oesteopath worked on trauma held within my body had regular bio resonance readings and homeopathic remedies – I also dealt with active tooth infections and removed a 20 yr old root canal treated tooth
I’m now walking 10-20 kilometres a day and still going with my health but I’m now plateaued with a constant stressed lymphatic system fatigue post nasal drip – my spine has been releasing from total a freeze to more flexible but shoulders hips sciatic nerve not great
I’m not in denial about the existence of these cavitations but more that the body can heal from anything if you put it in the right environment but there’s clearly something systemic still ongoing as I feel like I live with a co start low grade infection – I too have persistent ringing in the ears and blurry vision – my healing journey is not over and I do fear now that I will need to treat these cavitations in order to fully recover
I just know I had to be sure and at least after 2 years of healing im in a far stronger healthier position to have this surgery than I was before- im quite amazed that the biological dentists in the uk were happy to proceed with surgery when I was bedridden!
They advice should be get well prepare for the surgery so you have a way better chance of healing
I’m a completely different person health wise than I was 2 yrs ago as the brain fog was hideous back then and I couldn’t absorb all the information or research
So im still on a mission to chose the right surgeon to do my cavitational surgery in the uk as it seems pre and post operative care is paramount to the success
So far I’ve been to see biological dentistry lavender hill
Dr elmar Jung
NDU clinic london
There’s not many here in the uk not like in the us
Do you know of any biological holistic dentist in Michigan who does this type of surgery, and is trained?
I only know of Dr. Stuart Nunnally in Marble Falls, TX. He’s an excellent biological dentist with content on Youtube. Here are examples of his material:
https://www.youtube.com/watch?v=BlFM0TmU81c&list=PLmNM4HQYBO3pxYJh_BwVKjxwrH1cYbU-2&index=39&t=3318s
https://www.youtube.com/watch?v=fV20YaQ8WSg
https://www.youtube.com/watch?v=ZxBrdDQ96HA&t=1733s
I hope that you can find someone nearby, but if not, Dr. Nunnallly and his team are excellent alternatives. stay well.
Does anyone have any recommendations on the dentist that does cavitation in Florida or any states close to Florida?
I only know of Dr. Stuart Nunnally in Marble Falls, TX. He’s an excellent biological dentist with content on Youtube. Here are examples of his material:
https://www.youtube.com/watch?v=BlFM0TmU81c&list=PLmNM4HQYBO3pxYJh_BwVKjxwrH1cYbU-2&index=39&t=3318s
https://www.youtube.com/watch?v=fV20YaQ8WSg
https://www.youtube.com/watch?v=ZxBrdDQ96HA&t=1733s
I hope that you can find someone nearby, but if not, Dr. Nunnallly and his team are excellent alternatives. stay well.
Dr. David Edwards, Sanford Florida – had dental cavitation for my old wisdom teeth extract/dry socket last week and it went well. http://holisticdentalhealth.com/
Dr. Yolanda Cintron, Ft. Lauderdale Florida – she removed my mercury fillings in 2021.. https://www.gonaturaldentistry.com/dr-cintron/
Both are board member of IAOMT (International Academy of Oral Medicine and Toxicology)- https://iaomt.org/
For all of those asking, Dr. Carli Katz is an excellent Holistic Dentist in San Diego, very knowledgeable about cavitations / minimally invasive dental treatments. Here’s her info:
613 3rd Avenue Suite E
Chula Vista, CA 91910
619-489-1890
https://katzholisticdentistry.com/
This is great post and a valuable source for all.
Have any of you heard of Dr. Judson Wall in Utah? He has an impressive list of qualifications and is also an educator.
I would like to hear of experiences of those who have had dental cavitation surgery done by him.
My dental cavitations (from wisdom tooth extractions) and wisdom residual left in there have created years of problems for me. Including severe TMJ, trigeminal neuralgia and now eye issues. I am eager to have this surgery done by someone well qualified with a great track record.
I’ve been suffering from constant back ground facial neuralgia and jaw stiffness for 6 yrs.. all started with an overfilled root canal and a wisdom tooth w extraction that got infected.. I live in the Virginia Washington DC area and am looking for someone to investigate cavitations and the role they may be playing in my facial pain
Any help is greatly appreciated
do u think any testing is reliable for dental cavitations? Including Gum & dental socket infections etc? Looking into this it seems people tend to test negative even with conebeam but then they “treat it as if they have it” anyways and they find stuff.
Do u recommend any practitioners (even if they are online) who can interpret tests such as conebeam? TY!
Any biological dentists in florida thats experienced in cavitations?
Can anyone help me find a dentist who follows the Huggins-Grube protocol? I had root canals done years ago some of which are now painful. I cannot go to a regular dentist. I live in NH. Dr. Blanche Grube is not taking patients and I don’t know where else to turn.
Thank you
Holistic Dental Center in NJ.
https://holisticdentalcenternj.com/
91 Millburn Avenue,
Millburn, NJ 07041
973-379-9080
They follow the Huggins-Grube protocol and SMART Protocol.