 🖨️ Print post
🖨️ Print post
In 2019, the world discovered respiratory therapy, the profession that sprang out of World War II with the rise of jets flying into thin air at extremely high altitudes and studying the impact on the human body. As a registered respiratory therapist (RRT), I belonged (until my retirement) to that profession, which has grown and continues to change.
In 2020, during the height of the coronavirus, a new Covid hospital in the New Jersey Meadowlands (just west of New York City) begged me to come out of retirement, offering seventy dollars an hour—about twice the average hourly wage. I interpreted this request to mean that modern medicine was finally acknowledging respiratory therapists as the experts who know how mechanical ventilators interface with human beings. The fact is that nurses, as well as the pulmonologists and critical care physicians who prescribe this intervention, rely on the knowledge and experience that respiratory therapists bring to these critical situations.
Rather than return to clinical work, however, I now feel the best use of my twenty-five years of experience with ventilators in hospitals and home care is to share my knowledge and point of view with the public. Since many people have no understanding of the “how, when and why” of mechanical ventilation nor much awareness of associated ethical issues, the purpose of this article is to explain ventilator basics, especially as related to people with severe Covid. This may help you as you navigate the medical world on behalf of a loved one, or even yourself.
Purpose of Mechanical Ventilation
Mechanical ventilation is designed to do the breathing work for people with extremely disabled lungs. Usually, this is because of damaged lung tissue—as in chronic obstructive pulmonary disease (COPD)—or is due to extreme weakness of the surrounding muscles, as in neuromuscular conditions such as muscular dystrophy, post-polio syndrome or amyotrophic lateral sclerosis (ALS).
The ventilator pushes air into the lungs and then pauses for expiration (one breath); it then pushes another bolus of air into the lungs, and does this over and over again, either around the clock (if necessary) or for sleep and intermittently during the day.
Ventilators and Covid-19
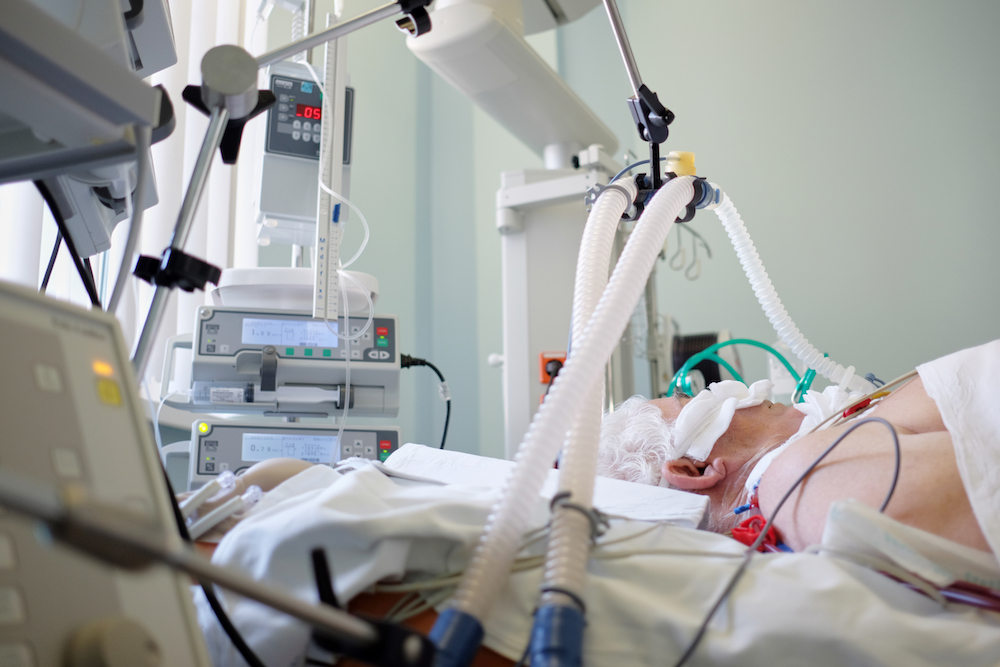
The lungs of critically ill Covid patients are connected to the ventilator in one of three ways—either with a tube inserted up the nose, or tube inserted into the mouth (these two are called “intubated”) or via a surgically created hole in the neck (this is called “trached”) below the voice box. All three procedures eliminate the possibility of speech and include sedation of one sort or another, especially when one is first intubated or trached.
It is important to know that there is a critical difference between the “usual” use of mechanical ventilation and Covid-related mechanical ventilation. The major difference is that the blood of many critically ill Covid patients lacks hemoglobin—iron to which oxygen attaches in the blood. Thus, while the ventilator continues to push in the bolus of air, creating the rise and fall of the patient’s chest, the blood is unable to accept the gift of oxygen. This may account for the low success rate of mechanical ventilation for people with Covid.
Preliminary research, published in May 2020, suggested this as an underlying reason for the failure of mechanical ventilation in Covid patients: “We speculated that in COVID-19, beyond the classic pulmonary immune-inflammation view [pneumonia], the occurrence of an oxygen-deprived blood disease, with iron metabolism dysregulation, should be taken in consideration.”1
Here’s my interpretation: severe Covid is basically pneumonia, accompanied, first, by a lack of hemoglobin (the oxygen-carrying particle of the blood) and second, by dysfunction of iron metabolism in the tissues. In the first case, the lack of hemoglobin means the blood is unable to transport oxygen—in other words, the blood cannot support life. The second feature (dysfunction of iron metabolism in the tissues) may cause blood clots, resulting in pulmonary embolism (PE) and/or deep vein thrombosis (DVT)—both potentially deadly.
Simply stated, in Covid, there is not enough iron in the blood and too much iron in the tissue, but scientists can’t say why.
The Essential Question
Here’s the essential question: Can ventilators truly support the life of critically ill Covid patients?
Let’s take a look at what the experts reported in one medical journal in January 2021. The American Journal of Respiratory Critical Care Medicine (AJRCCM), one of several journals published by the American Thoracic Society and publicly available online, reported a meta-analysis of sixty-nine studies that included outcomes for almost sixty thousand adult Covid patients following invasive mechanical ventilation. The bottom line, simply stated: The fatality rate for folks age forty or younger was 48 percent, and the fatality rate for patients over age eighty was 84 percent.2
Initially, this study’s findings suggested to me that invasive mechanical ventilation is pointless in the vast majority of Covid cases.
However, it is also important to remember that while we, the public, try to understand these critical medical issues, the medical community may be dealing with multiple issues and conflicting data, and definitions that can lead to misconstrued conclusions. In a July 2020 editorial, AJRCCM editor Hannah Wunsch, MD, argued that the medical community must learn how to report complex information with improved clarity and intention, stating “we need to. . . be vigilant in presentation of data to minimize confusion in interpretation.”3
So, what is the answer to the question about the use of mechanical ventilation with Covid patients? The science of iron in the blood and body tissues indicates that mechanical ventilation is not appropriate. The data from the AJRCCM meta-analysis lead to the same conclusion.

Now, the medical community is reaching for another high-ticket item—extracorporeal membrane oxygenation (ECMO) machines. The machine removes blood from the body via a tube placed in the neck, and then adds oxygen to the blood and pushes the blood back into the body. ECMO machines have been part of open-heart surgery for decades. However, while the demand for ECMO is high in the new Covid marketplace, the machines are in short supply.
More Questions
Here are some medical ethics questions: Who decides who receives high-priced equipment and associated supplies (and the trained personnel to go with them)? Who even wants this equipment? Are medical devices always used in the patient’s best interest? Are we pushing the inevitable—death—into an unsustainable future?
Your immune system is what keeps you healthy. There are thousands of microbes in our world. Some we can’t live without, while others may have the potential to cause great harm. How can you balance this and prevent disease?
From my vantage point as a health professional and a healthy and active septuagenarian, it is my immune system that allows me to live independently, disease-free, and to enjoy life. Thus, my daily task is to care for my immune system. I focus on my outbreath for energy as well as for management of pain and stress, and I include daily doses of nutritious food, water, exercise, restful sleep and joy—lots of joy!
What is your approach to the Covid conundrum?
REFERENCES
- Cavezzi A, Troiani E, Corrao S. COVID-19: Hemoglobin, iron, and hypoxia beyond inflammation. A narrative review. Clin Pract. 2020;10(2):1271.
- Lim ZJ, Subramaniam A, Reddy MP, et al. Case fatality rates for patients with COVID-19 requiring invasive mechanical ventilation. A meta-analysis. Am J Respir Crit Care Med. 2021;203(1):54-66.
- Wunsch H. Mechanical ventilation in COVID-19: Interpreting the current epidemiology. Am J Respir Crit Care Med. 2020;202(1):1-4.
This article appeared in Wise Traditions in Food, Farming and the Healing Arts, the quarterly journal of the Weston A. Price Foundation, Spring 2022
🖨️ Print post

My approach to the Covid conundrum is to eat what God gives us in nature and you won’t have to worry about your health. It is the only way to super-charge the immune system so that if you DO become ill the body easily overcomes it. 68 years old, I’ve been doing it for years. I don’t get sick. No chronic conditions, no aches or pains. Man’s garbage, so-called “food” kills you slowly.
What the medical establishment claims to be viruses, are manifestations of our own bodies that happen when there’s an insult. They are a reaction to toxins, a defense mechanism. They are not the cause of illness but the solution, created inside and by the body to solve a specific problem and they’re not transmissible.
We know they’re not transmissible because scientists tried to infect healthy people with the Spanish flu using fluids from the sick. They squirted the fluids in the nose, throat and even injected it. The healthy did NOT become ill.
So the idea of a virus as an infectious particle in the air or fluids causing infection and illness is false. That does not exist. At the very least, decent science to prove the notion, does not exist.
There are microbes, there are bacteria, but “viruses” do not exist in Nature. “Viruses” only exist as a set of symptoms inside the body, as a result of an acidic pH imbalance.
This is what the scientists who claim to have isolated a virus would likely do: They take a dying, rotting and decaying Green Monkey kidney tissue cell in a virologist’s Petri dish that has been starved of nutrients, poisoned, broken down and decayed further with antibiotics like Gentamicin, Amphotericin, Phenol Red acid dye and kidney dissolving Trypsin enzymes from many days, then poisoned further with fixitive neurotoxic preservatives like Formalin, Formaldehyde, Gluteraldehyde and then de-hydrated in alcohol baths of Ethanol and Acitone, then put into a mold filled with epoxy glue and wax, then frozen and sliced into micro thin pieces, then stained with heavy metals made of Lead and Uranium acitate and then bombarded with 150 degrees to 300 degree celcius heat beams under an electron microscope to show a picture of a still, non moving piece of cellular debris which virologists label a “virus” particle. So what IS this particle? It is a theoretical guess based on electron microscope pictures that have been put through all of the ludicrous chemical procedures just described. They are just artist drawings and computer-generated pictures of what virologists THINK that black and white 2-dimensional image might really look like. Nobody has ever seen one. It’s imagination only.
https://odysee.com/@dharmabear:2/The-End-of-Germ-Theory-Spacebusters-doc-2022:d